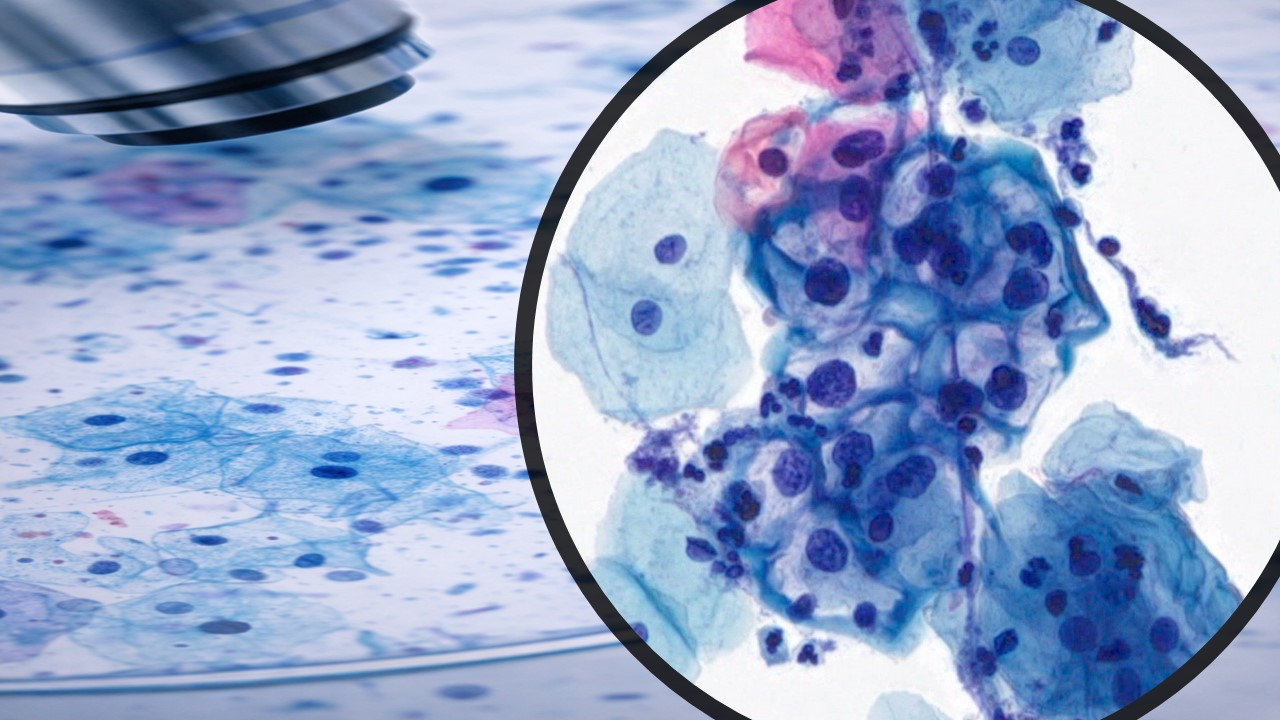
BODY CAVITY FLUIDS CYTOLOGY
The pleural, peritoneal, and pericardial serous cavities, usually referred to as body cavities, are lined by a single layer of mesothelial cells and, in the healthy person, contain very little fluid. Serous effusions occur when fluid, either as a transudate or exudate, accumulates in the cavities. Transudates have a low protein content and specific gravity and are mostly caused by cirrhosis or congestive cardiac failure. Exudates, in contrast, have a high protein content and specific gravity. They have a broader etiology and include inflammatory, neoplastic, connective tissue, and iatrogenic disorders. Serous effusions can occur at any age and may be the initial presentation of the disorder or a later manifestation. Most serous cavity-fluid specimens are effusions, but some are obtained by using a saline wash to exfoliate cells from the mesothelium.
Cytologic examination of the cellular features of fluids is a valuable adjunct to patient diagnosis and the staging and management of tumors, in particular, gynecologic tumors.
SPECIAL INSTRUCTIONS FOR THE COLLECTION OF BODY CAVITY FLUIDS
When a large volume of fluid (greater than 1000 mL) is obtained, allow the cellular material to settle in the bottom of the collecting container, and then gently pour off the excess supernatant. Agitate the remaining fluid to resuspend the sediment and pour into an appropriate specimen container. In general, the quantity of specimen sent should not exceed 800 mL.
Submit the specimen in a tightly covered glass or hard plastic container with a screw-top lid. Volumes of fluid 200-800 mL may be submitted in brown plastic 24-hour urine collection containers. Soft plastic collection bags and E-Vac containers with clamped tubing ARE NOT ACCEPTABLE for submitting body fluids for cytologic evaluation. They are difficult to handle for processing and tend to leak in transit, which can cause contamination of the tube system as well as causing a health hazard to hospital and laboratory personnel. Secure the specimen for transport at the site of collection to avoid accidents.
Refer to the earlier section on submitting specimens to the Cytology Laboratory for additional information regarding applicable procedures for specimen collection and submission.
Health Tips
Which submission form do I use?
A filled out Cytology Submission Form must accompany all effusion (body cavity fluid) specimens for cytology
What are the components of a “full fluid analysis” (“centesis fluid exam”)?
Full fluid analysis includes total protein (TP, using a refractometer), total nucleated cell count (TNCC, using a
hematology instrument), and cytologic evaluation.
The appropriate specimen to submit is fluid in a sample tube smears you have made. Fluid cytology specimens should be ordered as “Centesis Fluid Exam and Report” (if cavity effusion) OR “Synovial Fluid Exam and Report”(if synovial fluid). For full fluid analysis of synovial fluids, one accession is required per anatomic location.
What collection tube should I use?
For ALL fluid specimens for cytology (pleural, peritoneal, and pericardial effusions and joint fluids)*, place the sample into an EDTA (lavender-top) tube.
EDTA will prevent clotting and preserve cells for cytologic examination.
Fill EDTA tubes to the fill line.
The fill line is indicated by a small line or mark on the tube label. Under-filling the tube will cause falsely high total protein results. Over-filling the tube creates a risk of clotting.
Do not use expired sample tubes.
Expired tubes may contain ineffective anticoagulant or have lost their sterility
What if I don’t have enough fluid to properly fill an EDTA collection tube?
If you do not obtain enough fluid to correctly fill an EDTA tube, but you have enough fluid to make a few direct smears, do so and submit the smears as “Cytology Smear Evaluation and Report”.
For synovial fluid, if you are submitting smears only, you may submit fluid smears from up to three joints as one accession.
What other testing can I do with body cavity fluids?
If you also want to submit fluid for culture, place an aliquot into a clot (red-top) tube. Clot tubes have no fill line and sample volume is not critical.
Please note that fluid specimens for culture go to the Clinical Microbiology Laboratory (not the Clinical Pathology Laboratory).
If you also want to perform chemistry testing on fluids, either a heparin (green-top) tube or a clot (red-top) may be used.
Heparin tubes should be filled to the fill line, and specimens should be accompanied by a filled out ClinicalPathology Submission Form.
Is fluid in a tube all you need? Should I make smears?
If you have enough sample, always submit fluid in a properly-filled EDTA tube. This allows us to give you a TP and TNCC along with the cytologic evaluation and allows the pathologist to make as many extra smears or cytocentrifuge preparations as needed.
We recommend also making one or two direct smears of fresh fluid at the time of sampling.
Smears can be made using a “blood smear” technique, air-dried, and placed in a slide holder.
If the fluid looks very clear and you have enough sample, consider making a concentrated preparation of the fluid at the time of sampling.
Use the same procedure as you would for making an air-dried preparation of urine sediment.
Be sure to label the resulting smears as “concentrated”, so the pathologist is aware!
How do I store and ship fluid samples?
EDTA tubes should be refrigerated at 4 to 5 C. If mailed to the laboratory, these should be sent by overnight mail on an ice pack.
Slides should NOT be refrigerated. Slides may be shipped in the same box as the EDTA tube, but protect slides from moisture and keep away from the ice pack.
Specimens transported to the UTCVM should be dropped off at the laboratory sample submission area in the hallway outside pharmacy (large animal hospital side). You may wish to leave a note with any EDTA tube (in refrigerator) whether slides accompany the specimen, and you may wish to leave a note with any slides (in the cytology drop-off box) that there is accompanying fluid and a submission form in the refrigerator.
How do I properly label fluid tubes and smears?
All specimens must be labeled using two unique patient identifiers. E.g., patient name and owner name, or patient name and medical record
Each specimen must be individually labeled. E.g., multiple specimens taped together with one tape label are NOT acceptable and will be rejected by the laboratory